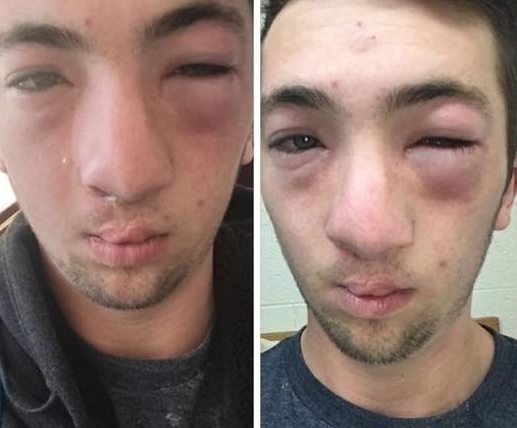
Updated: February 2024 – After using an epinephrine auto-injector for anaphylaxis, patients have been told for years to call 911 and go to the emergency room.
But new guidelines for allergists say that in many cases, it may be safe to stay home. Those situations include when symptoms of the allergic reaction quickly go away after using an epinephrine auto-injector. The stay-home advice would be aimed at patients who have a second epinephrine auto-injector on hand, in case symptoms return.
“If the patient has used epinephrine promptly, and has prompt, complete, and durable response to treatment … they don’t really need to call EMS or go to the emergency department,” says Dr. David Golden. He’s a co-author of the revised guidelines, called the 2023 Anaphylaxis Practice Parameters Update, which were published in February 2024.
So why this major change? The allergists on the task force who wrote the updated guidelines say that linking use of an auto-injector with having to call 911 has led to hesitation to use epinephrine in serious reactions. Some people have avoided using epinephrine because they don’t want to go to the emergency department.
In situations where anaphylaxis symptoms resolve quickly with epinephrine, there isn’t much for doctors at the ER to do for patients anyway, says Dr. Marcus Shaker, a professor of pediatrics and medicine at the Geisel School of Medicine at Dartmouth.
“Needing to activate EMS created a barrier to epinephrine use for families,” says Shaker, a co-chair of the joint task force on the practice parameters.
“More often than not, what would happen is patients with resolved anaphylaxis would incur ambulance and emergency department costs, accompanied by prolonged and inconvenient hours waiting in an emergency department, all to be discharged without any additional intervention.”
ER After Epi: Severe Symptoms
The experts stress there are still plenty of situations when anaphylaxis symptoms do mean it’s best to head to the emergency department. Patients should still call 911 if anaphylaxis symptoms are severe. They should also call 911 if the symptoms of their allergic reaction don’t go away completely (or nearly completely). They should also call 911 if symptoms start to come back.
“We recommend absolutely to activate EMS if the reaction is severe, or fails to resolve promptly or starts to return,” says Golden, an allergist-immunologist and associate professor at Johns Hopkins University in Baltimore.
The new guidance stresses the importance of immediate access to a person who can provide help, should the patient need it.
The new practice parameters were developed by a task force representing the American College of Allergy, Asthma and Immunology (ACAAI) and the American Academy of Allergy, Asthma and Immunology (AAAAI). Highlights were presented at the 2023 ACAAI annual meeting in California.
Worries about Biphasic Reactions
Traditionally, food allergy and anaphylaxis action plans, like this one from FARE, have recommended that allergy patients be transported to the ER after getting epinephrine, “even if symptoms resolve.” The patient should then “remain in the ER for at least four hours because symptoms may return.”
Shaker says many allergists gave that recommendation, and that it related to concerns about the risk of biphasic reactions. That’s the reoccurrence of symptoms hours after the first symptoms have passed.
But newer research shows that biphasic reactions aren’t all that common. About 98 percent of allergic reactions get better after one or two doses of epinephrine. And one meta-analysis found that fewer than 4 percent of reactions reoccur.
Allergists were finding that their “abundance of caution had unanticipated consequences,” Shaker says.
Getting patients or caregivers to use epinephrine promptly was the ultimate goal. Yet telling families that they should always call 911 after auto-injector use sent a message that epinephrine is a dangerous medication, says Dr. Julie Wang, a professor of pediatrics and allergy at Mount Sinai Hospital in New York.

In a survey that she and her colleagues conducted, about 4 percent of parents specifically cited not wanting to call 911 or go to the ER as a reason for not using the auto-injector when symptoms called for it. As well, 7 percent said they were worried about the epinephrine itself. (Epinephrine is in fact very safe to use in most patients.)
“We have noticed in practice that families tie the two points. ‘Once I use epi, I have to call 911.’ They think ‘epinephrine is dangerous enough that I need to call 911’. Or, ‘if I don’t want to go to the ER, I should not give epinephrine,’” Wang says.
ER After Epi: When Else to Go
Even when anaphylaxis symptoms appear relatively mild, the experts note there is still much to consider when deciding whether to call 911 or not.
To start with, the new recommendations apply specifically to the home, Wang says. If anaphylaxis occurs at a school, the recommendation will still be to call EMS.
Even inside the home, if a child or adult is home alone, or a long distance from a hospital, call EMS. The updated guidelines say to do the same if the patient has a history of severe or near-fatal anaphylaxis. (Examples are those whose previous anaphylaxis had to be treated with more than two shots of epinephrine, hospitalization and intubation.)
Patients experiencing an allergic reaction should never feel that they shouldn’t call 911 and go to the ER, Wang stresses. “This is not intended to make anyone uncomfortable. If somebody wanted to call EMS, they absolutely should call EMS.”
Physicians and patients with allergies need to discuss their plan and make decisions together, she says. This should include making sure they have at least two auto-injectors on hand, are comfortable with using them, and recognize the symptoms of anaphylaxis.
“If a teen was home alone and having anaphylaxis and had self-administered,” waiting at home might not be a good idea, Wang says.
Costs of ER after Epi
Wang, Golden, Shaker and the other practice parameter authors also weighed the costs of ER visits for anaphylaxis symptoms that had resolved.
Patients and insurers pay for the ambulance transport and fees for being observed for hours in the emergency department. A 2019 study by Shaker and colleagues examined the costs of using the ER for medical observation after peanut allergy reactions that were treated and promptly resolved. They concluded there was “minimal benefit and excessive costs.”
Shaker says that during the COVID-19 pandemic, “the low value proposition of waiting in an emergency department for several hours when you don’t have symptoms really became clear. The risks of infection made us consider how much benefit patients were getting out of this kind of observation.”
The Canadian Society of Allergy and Clinical Immunology recently adopted guidelines similar to the task force parameters on home management of food-induced anaphylaxis without calling EMS.
Will This Boost Auto-Injector Use?
One hoped for change of not insisting on automatic transport to the ER is encouraging more people to use epinephrine auto-injectors when needed. Epinephrine auto-injectors are the best treatment for halting severe allergic reactions. Yet people often hesitate to use them.
“The most positive thing about this change is it will likely encourage people to use epinephrine and use it early because they won’t feel they have to go to the ER if they use it,” notes Dr. James Baker, director of the Mary H. Weiser Food Allergy Center at the University of Michigan.
The updated parameters are to be published in an upcoming issue of the Annals of Allergy, Asthma and Immunology.
Related Reading:
Inside the Epidemic of Epinephrine Hesitation
Allergic Living’s ‘All About Epinephrine’ Guide