An expert panel has recommended that the U.S. Food and Drug Administration approve a new, epinephrine nasal spray for treating severe allergic reactions.
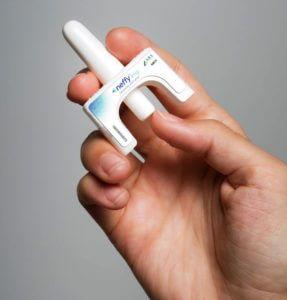
If the nasal spray – called neffy by ARS Pharmaceuticals – is approved, it would become the first needle-free epinephrine device.
The 22-member advisory committee voted on May 11, 2023, that the safety and efficacy results from ARS Pharma’s clinical trials were sufficient to recommend neffy’s approval for adults and children weighing 66 pounds or more.
The panel voted 16 to 6 to recommend approval of the 2-milligram epinephrine spray for adults, and 17 to 5 to recommend it for children. The FDA, which often follows the recommendations of its expert panels, is expected to make its decision in mid-2023. [Update: In June, the FDA extended its review deadline until September 2023.]
Several of the experts who voted in favor of the nasal spray reminded their colleagues of the families and patients with food allergies. During a public comment period, parents and teens spoke emotionally about terrifying experiences with anaphylaxis and with auto-injector fears. They also spoke of the relief they’d feel having a needle-free option to treat allergic emergencies.
‘Huge, Unmet Need for Patients’
The data “do indeed support a favorable benefit-risk assessment,” said Dr. Paul Greenberger, an emeritus professor in the division of allergy and immunology at Northwestern University’s Feinberg School of Medicine in Chicago. “Let’s keep focused on the huge unmet need that we heard about and we know. Anything to get epinephrine into people, effectively and faster, the better.”
Dr. John Kelso, an allergist at Scripps Clinic in San Diego, also voted to approve neffy. “The data showed the drug gets into the bloodstream and has an effect in a way that’s comparable to injectable products that we are using now, and I have no reason to think it wouldn’t have the desired clinical outcome,” Kelso said.
However, some who voted against the novel product noted there was no real-world clinical data on nasal epinephrine. (For ethical and safety reasons, all studies were done in healthy volunteers not having allergic reactions.)
They also pointed to data from ARS Pharmaceuticals showing that it takes a few minutes longer for nasal epinephrine to reach peak concentration in the blood compared to epinephrine injected into the muscle using an auto-injector.
Those first 10 minutes, when clinical trial data showed that thigh-injected epinephrine was absorbed faster than nasal epinephrine, is a “really critical period,” said Dr. Bridgette Jones. The professor of pediatrics at Children’s Mercy Kansas City in Missouri also questioned if kids would necessarily be more likely to carry or use a nasal spray.
But other experts felt that the 10-minute time period was somewhat arbitrary. Other data from the first moments – such as increases in heart rate and blood pressure – showed the nasal epinephrine was being rapidly absorbed.
They also noted that if people are more willing to use the nasal spray, cutting down on delays might more than make up for any differences in absorption rates.
“Even though there is some uncertainty about the first 10 minutes .… we need to consider the time to dosing with this method and take that into the full discussion,” Dr. Janet S. Lee said. Lee, the director of the division of pulmonary and critical care at Washington University School of Medicine in St. Louis, voted in favor of approval.
Families Urge Needle-Free Epinephrine
Epinephrine is a lifesaving medication for people with allergies to food, medication or insect venom. But epinephrine must be given promptly. Delays tend to mean worse reactions, or needing more than one dose.

Surveys have shown again and again that many people fail to use epinephrine auto-injectors, even when symptoms call for it. Some find the pen-style devices inconvenient to carry. Other reasons for the reluctance include needle fear and panic when an anaphylactic reaction occurs.
The FDA received over 600 online public comments on the epinephrine nasal spray. Many food allergy parents wrote to say that a nasal spray was potentially “life-changing.” They urged the FDA to approve the ARS device.
During public comments at the meeting, some parents related distressing experiences of having to hold down their struggling child to administer the auto-injector. Or of having their child jerk away from them when they tried to give them the needle. They talked about their children developing needle phobias after needing an auto-injector multiple times.
Amanda Bee’s daughter, Vivian, 11, has food allergies to dairy and beef. Despite being an experienced food allergy mom and advocate, she’s had to use give her child auto-injections nine times. Her daughter has become fearful and anxious of the injector, and now will hide her symptoms to avoid the shot.
“It took the strength of me and my husband both to hold her down and inject her with epi,” Bee said of one incident. “The treatment is feared as much as anaphylaxis,” said the Utah mother, adding that a nasal spray alternative would help her as well as her daughter.
Patients and Needle Resistance
Jared Saiontz, a 15-year-old with 26 food allergies, talked about his dread with having to use the auto-injector during a recent allergic reaction. He was finally able to do it – only with the help of his brother. His brother steadied his hand as they injected the auto-injector together. “If we can get this nasal epinephrine …. I know it’s not going hurt, and I know my life is just going to be saved,” he said.
Speaking in favor of neffy, Dr. John Oppenheimer, clinical professor of medicine at UMDNJ Rutgers University School of Medicine, noted the safety and efficacy of epinephrine auto-injectors is well-established. However, “a large majority of our patients and their caregivers struggle to use these bulky, needle-bearing injection devices.”
“They fail to fill the prescriptions, carry their devices and are hesitant to use their devices during an allergy emergency due to needle phobia or fear of adverse reactions,” he said.
Richard Lowenthal, ARS Pharma’s president and CEO, thanked the panel for their support and robust discussion. As for the allergy families, he said: “we were moved by the outpouring of support for neffy ahead of and throughout this meeting.” He expressed particular gratitude to “those individuals who shared their personal experiences, illustrating the positive impact neffy may create for millions … in the future.”
Neffy’s Study Data
The company’s new drug application was based on data from four studies. Lowenthal told the panel that the data show that neffy’s efficacy falls within the range of other epinephrine products, including EpiPens and manual epinephrine given by syringe.
So far, neffy has been tested on more than 600 adults and children in clinical trials. Any adverse effects have been mild. No serious adverse events were reported in any clinical study. (The company is also testing a 1 mg dose for children 33 to 66 pounds. It plans to submit those results to the FDA if the current application is approved.)
With neffy, as with other epinephrine products, for safety the trials are not conducted in people having actual allergic reactions. Instead, researchers use healthy volunteers and then measure changes to heart rate and blood pressure. If those go up, this indicates the epinephrine is being absorbed.
Clinical trials also measure peak concentration of epinephrine in the blood, and how long it takes to reach the peak after being given epinephrine. This is compared to already approved methods.
Neffy in Stuffy Noses
The company also conducted a clinical trial looking at how well the nasal spray works in those with stuffy noses.
Researchers exposed study participants to an environmental allergen, to cause to nasal congestion. That study found that a stuffy nose actually led to faster absorption of the epinephrine. The investigators suspect this is because the mucus membranes become more permeable when there is congestion. However, the concentration of epinephrine fell more quickly.
“Congestion accelerates the absorption,” Lowenthal told the committee, whereas a runny nose causes the medicine to drain out of the nose more quickly.
The FDA has approved Neffy’s sprayer device for drug delivery for six other drug products in the United States. Many are intended for emergency use.
The minority of experts who voted against recommending the nasal spray said more data was needed on how the medication would perform during actual allergic reactions.
But the majority said there is no safe or practical way to test new epinephrine products in those experiencing anaphylaxis. “In the end, I felt the benefits outweighed the risks,” said Dr. John Tracy, a clinical professor of pediatrics at University of Nebraska College of Medicine.
Related Reading:
Earlier Article: Epinephrine Spray, Film: How Do They Work?





