
Updated May 12, 2023 – A needle-free alternative to the epinephrine auto-injector has taken a crucial step forward with the U.S. Food and Drug Administration.
The FDA has accepted a new drug application for an epinephrine nasal spray. ARS Pharmaceuticals developed the spray, known by the brand name “neffy”. A new drug application is a formal request by a pharmaceutical company to approve a new medication. It includes all the clinical data that a company thinks it needs for approval.
The FDA scheduled an advisory committee meeting for May 11, 2023, where a panel of experts reviewed the data on neffy. [Update: Allergic Living’s report on that meeting is here.]
The results of the FDA’s review are expected in September 2023, says Richard Lowenthal, co-founder and CEO of San Diego-based ARS Pharmaceuticals. Epinephrine is the essential drug for halting severe allergic reactions. If approved, neffy would be the “first new way of delivering epinephrine in over 30 years,” Lowenthal says.
In their application, the company asks the FDA to approve a 2 milligram (mg) dose for use in adults and children weighing 66 pounds or more. That dose could be repeated a second time if needed.
The company is also testing a 1 mg dose for children under 66 pounds. It has plans to submit those results to the FDA in mid-2023.
As second half of this article will reveal, headway is also being made with other needle-free epinephrine products. This includes an epinephrine film that dissolves under the tongue.
Looking for Auto-Injector Alternatives
Epinephrine auto-injectors are known to be very effective in stopping anaphylaxis, when given promptly. Yet, studies show auto-injectors are often not used or, despite symptoms, they’re administered after delay.
In a 2021 survey, Mount Sinai researchers analyzed why parents didn’t use an auto-injector when a child was having a severe allergic reaction. The top reasons included not recognizing symptoms as severe enough or feeling nervous about using the auto-injector.
In its research, ARS Pharma provides data to suggest a nasal spray could help overcome some reluctance to use epinephrine.
The company surveyed 200 patients and caregivers who had used an epinephrine auto-injector in the past year. Forty percent of respondents said they delayed use of the auto-injector by an average of 8.8 minutes from the time symptoms started.
The top reasons given for the delay: uncertainty about whether initial symptoms warranted use of the device, needle fears, the recommendation to go to the ER after using the device, concerns about potential side effects from epinephrine, worries that the auto-injector would be painful or hit bone, and the size of the device.
When offered the hypothetical choice of using a needle-free delivery device instead, survey respondents said they would be more willing to use it. They also said they’d use it faster.
“A needle-free option for administering epinephrine would be used sooner after symptoms developed and is perceived as being easier to use versus an injectable device,” the company stated.
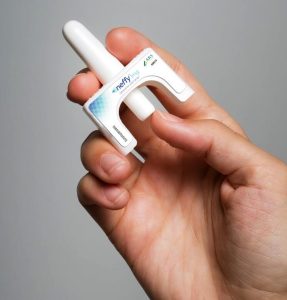
Kids and adults also said they would be more likely to carry the nasal spray. If approved, the company plans to package two neffys in a box. Together, they’re about 2.5 inches by 1.7 inches in a pocket – about the size of an earbuds case.
Epinephrine Spray: How Well Does It Work?
Clinical trials of epinephrine products – including the various brands of auto-injectors – are conducted using healthy volunteers, not people having actual allergic reactions. This is for safety and ethical reasons, notes Dr. Harold Kim, an associate professor at Western University in Ontario, Canada, and chair of the immunology and allergy division. (Kim is not involved with research into the auto-injector alternatives.)
Instead, when testing new epinephrine delivery methods, researchers measure heart rate and blood pressure, which should go up as the epinephrine is absorbed.
They also measure the peak concentration of epinephrine in the blood, and how long it takes to reach the peak.
Data from ARS Pharma included an analysis of 59 healthy adult participants. They were given either the 2 mg nasal spray, a 0.3 mg manual injection of epinephrine to the thigh muscle, or a 0.3 mg EpiPen.
The study found that following a single dose, it took 7.5 minutes to reach peak concentration in the blood with the EpiPen. Neffy took 30 minutes, while the manual injection took 45 minutes.
EpiPen also had the highest peak concentration, followed by neffy, and then manual injection. Additionally, EpiPen also had the highest average concentration levels until 20 minutes. But starting at 30 minutes, the nasal spray had higher average concentrations.
Blood pressure and heart rate increased using all three delivery methods, but remained elevated for longer with the neffy.
Researchers say the action of neffy is “within the range of currently approved epinephrine products.”
“These results demonstrate that neffy has the potential to be a safe, effective, and more convenient alternative for the emergency treatment of … anaphylaxis,” the company concluded.
Epinephrine Spray and a Stuffy Nose
ARS Pharma also conducted a similar test in people with allergic rhinitis. They found that having a stuffy nose due to seasonal allergies led to more rapid absorption of epinephrine; the time to maximum concentration was 6 minutes. However, the peak level was about 35 percent lower than in people with clear nasal passages. (The company says this is still within the acceptable range for approved epinephrine products).
In reviewing the company’s results, Kim said the overall levels of epinephrine in the blood after the nasal spray are on par with auto-injectors – although it may take longer to get there. “It shows the nasal approach leads to good serum levels,” he says, noting that the nose is very efficient at absorbing medications.
However, the “delayed peak in levels is a little bit concerning because of course we want to treat anaphylaxis immediately.”
And yet, if people are more willing to use an epinephrine nasal spray, and less likely to delay using it, that could make a slower response less of an issue, he adds. “The huge benefit of this drug is it’s not a needle, and it may be much easier to convince patients to use it,” he says.
Prior research has shown that auto-injectors take about 5 to 10 minutes to reach peak concentration, which is about what the ARS Pharma research found.
However Kim, who’s a past-president of the Canadian Society of Allergy and Clinical Immunology, says some of the results are unexpected. He was surprised that manual injection took 45 minutes to reach the peak. Manual injection is how emergency departments administer epinephrine. “We don’t have any evidence to suggest an auto-injector is better than an intramuscular injection,” notes Kim.
If the nasal spray is approved, he expects physicians and many families with food allergies will want to see real-world evidence that the nasal spray halts severe allergic reactions as well as auto-injectors.
For instance, he might first try the nasal spray in patients having mild reactions during food challenges, until he’s sure it works as well as an auto-injector.
Dissolving Epinephrine Makes Strides

Another needle-free epinephrine alternative is also making progress. Aquestive Therapeutics has wrapped up their Phase 2 trial of an epinephrine film that dissolves under the tongue, and the results look promising.
In a study comparing the sublingual film to 0.3 mg EpiPen or 0.3 mg manual injection, they found the time to maximum concentration was fastest with the dissolving film at 12 minutes. The EpiPen took 22 minutes, while manual injection took 45 minutes. (Kim says that there can be variability in epinephrine response times, which is why allergists want us to get enough of it fast in anaphylaxis.)
“Where we think our product really shines is you get a lot of absorption very quickly. Our median time to peak concentration is 12 minutes. We think that is the most critical thing in this particular disease state, because you are trying to stop the cascade,” says Dan Barber, CEO of the Warren, New Jersey-based company.
Aquestive plans to launch their Phase 3 trial in late summer 2023. It plans to complete the trial in mid-2024, and submit for approval in 2025.
For the Phase 3 trial, the FDA has asked Aquestive to compare their film to EpiPen and two other brands of auto-injectors. “We definitely feel positive. We think this was an important step forward and we think it’s bringing us even closer to our filing,” he says.
“The FDA does appear to be committed to getting an alternative delivery product out there or multiple alternative delivery products out there, which is refreshing,” Barber says.
UTULY Nasal Spray Candidate
Another contender in the needle-free epinephrine category is Bryn Pharma’s UTULY nasal spray. Last fall, the North Carolina company reported a positive comparison study for its UTULY 6.6 mg epinephrine nasal spray versus the 0.3 mg EpiPen.
In their most recent research, the company reports that two doses of the nasal spray – a total of 13.2 mg of epinephrine – tested in 100 healthy volunteers reached peak concentrations that were higher than the auto-injector. The maximum concentration was also reached more quickly.
The data were revealed in a poster presented at the 2023 American Academy of Allergy, Asthma & Immunology (AAAAI) meeting in San Antonio.
Bryn also sounds confident in moving forward to an FDA review. “Our findings have given us the confidence to move forward in the regulatory process,” says CEO David Dworaczyk, PhD.
Related Reading:
Anaphylaxis But No Epinephrine: An Epidemic of Hesitation
All About Epinephrine, with ER Dr. Julie Brown
At 30,000 Feet, Why We Can’t Count on Epinephrine Vials on an Airplane





