
Back in 2016, the food allergy community had high hopes for a bipartisan Senate bill that would have required all U.S. airlines to carry epinephrine auto-injectors on every flight, and to train crews to use them. But the proposed law failed to pass.
Then in the summer of 2019, two high-profile reactions occurred on airplanes, involving stories of difficulty either accessing epinephrine or getting an additional dose of the lifesaving drug. This has given a renewed sense of urgency to lobbying to get epinephrine auto-injectors into airline emergency kits. From a few senators to physicians, proponents like the non-profit FARE and advocates including me, all of us have been urging this change.
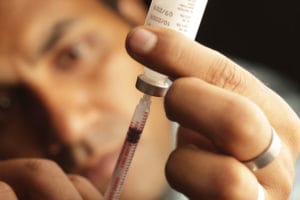
Experience shows that epinephrine vials and syringes are harder to use in-flight than an auto-injector. Plus, such a shot can only be given by a medical professional.
But now it turns out, there is no guarantee that even an epinephrine vial will be on your next flight. In fact, if you forgot your auto-injector or needed an extra dose, you could be 30,000 feet in the air without any epinephrine.
Flying under the radar has been the fact that Airlines for America, the carriers’ trade association, asked the Federal Aviation Administration (FAA) for a four-year exemption for its members in times of drug shortages. The FAA approved the the exemption in 2016, which permits most large carriers to fly planes without up to five drugs normally required in their kits, if a supply issue arises. Two of the medicines are epinephrine – in differing doses for either anaphylaxis and heart attacks.
Exemption’s Red Flags
Illinois Senator Tammy Duckworth, working alongside New York Senator Chuck Schumer on the auto-injector issue, learned of the exemption late in the summer of 2019. Her staff discovered it in FAA documentation, and realized this meant some airlines may not be carrying epinephrine – even in vial form.
“No traveler should ever fear that an allergic reaction on a flight might go untreated because the airline was quietly granted an exemption from carrying lifesaving medications like epinephrine,” Duckworth told me by email. She and Schumer are calling on the FAA and the airlines to review the policy – and to work toward getting epinephrine auto-injectors on flights.
Even knowing which airlines have been granted an FAA drugs exemption is not helpful to the allergic flyer. What is clear to me is that we still have NO idea how many emergency kits on airlines’ planes are missing epinephrine.
The situation raises troubling questions, such as did the FAA consult physicians in making the decision to grant individual exemptions, and how do they verify there is no abuse of the exemption policy? The health-system pharmacists’ group ASHP says cardiac epinephrine pre-filled syringes are currently in short supply, but vials in other dose strengths are available.
There is no epinephrine vials shortage as such. But what we don’t know: when a supply issue ends, how soon are medical kits restocked?
The FAA’s decision states that exemption holders “must refurbish the missing drugs at the next scheduled refurbishment date.” But how would a passenger or a physician called to assist in an emergency know whether the drugs have been refurbished on a plane – or not? There is no way to access the information that would how many planes in the air, and which ones, don’t have epinephrine on board.
American Airlines and Southwest Airlines have both told CBS News that their emergency kits are stocked with the required epinephrine. That is good to know, but the FAA exemption still shrouds this “requirement” in a fog. Are passengers expected to poll every airline customer service center about the kits, and would their representatives even know?
Epinephrine Incidents in the Air
The New York Times investigated the airline drug exemptions situation. FAA officials told the Times that “passengers ought to be aware of the exemptions, since the request process is public, and all decisions are posted on the Federal Docket Management System.”
This statement is absurd. The average passenger is not even aware of FDMS, let alone how to navigate it. More evident is the critical need for in-flight epinephrine. Consider these cases:
• Dr. Mikhail Varshavski, known on social media as “Dr. Mike,” this summer assisted a passenger on a flight from New York to Tel Aviv. The man, who was suffering anaphylaxis, had no history of allergies and did not carry an auto-injector. In the airline’s medical kit, Varshavski found an epinephrine vial with the concentration for a heart attack. He had to troubleshoot correcting the dosage on “the fly”. The man recovered.
• In May 2019, Harvard student Alexa Jordan began to have an anaphylactic reaction to a purchased salad. In her case, which attracted national television coverage, she used her own auto-injector. Jordan says she was offered no further epinephrine or assistance in a reaction in which she was passing out.
• In February 2018, nurse Kellie Hopkins got a flight crew to poll passengers for an available auto-injector while attending a 10-year-old having a severe, first-time reaction. She did not feel she had time to look up the dosing for a child when using a vial.
• In May 2018, Ashley Spencer had a life-threatening anaphylactic reaction aboard a flight to Cleveland. Doctors who stepped forward administered her two epinephrine auto-injectors, but she needed more. One doctor who tended to her simply grabbed an auto-injector from his personal kit.
In anaphylaxis, “there’s really no substitute for prompt administration of epinephrine,” notes Dr. David Lang, president of the American Academy of Allergy, Asthma and Immunology and chair of the allergy department at the Cleveland Clinic. “Delay in its administration, as well as lack of administration, have clearly been implicated in a number of studies as a risk factor for more serious anaphylaxis, and even fatal anaphylaxis.”
That risk hits home for Houston allergist Dr. Patricia Leonard. In 2014, she assisted a 4-year-old suffering a fast-moving anaphylactic reaction – which began two hours into a transatlantic flight. “In less than five minutes of consuming a cashew nut, the girl’s symptoms progressed to a severe, life-threatening reaction,” Leonard recalls.
Epinephrine stopped the child’s first-ever anaphylactic reaction. “If she did not receive the epinephrine, I would assume that her condition would have continued to deteriorate,” says Leonard.
Asked about the FAA exemption, she says: “Epinephrine is a basic lifesaving medication. Passengers should expect the airlines to stock basic emergency medications on each flight.”
Questionable Data
In a June 2019 report to Congress regarding allergic reactions aboard aircraft, the FAA cited a 2013 study that found only 2.2 percent of medical events on aircraft are due to allergic reactions. But the agency’s letter goes on to state: “There are currently no regulations or statutes that require airlines to report to the FAA about allergic reaction events on aircraft. Additionally, the FAA does not track any reports it might receive about such events.”
So in truth, there is a lack of data about allergic reactions in the air. For example, serious medical emergencies are not necessarily declared while in the air. An incident in which a passenger becomes seriously ill on a plane and then receives medical treatment after landing may only be recorded in relation to the on-land treatment.
Retrospective studies have shown that allergic reactions in the air are often not reported to airline staff. Plus anecdotally, my airline advocacy website continues to receive many testimonials asserting anaphylaxis in the air. Simply put, there is an urgent need for better tracking of allergy incidents.
At a minimum, ensuring epinephrine vials are on all airplanes could mean the difference between life and death for a food-allergic person, or the passenger who does not yet realize they have an allergy. In schools, data show that 25 to 30 percent of stock epinephrine is administered to students whose allergy was previously unknown.
Agency Has Scope to Act
Back in 1984, Ralph Nader’s Aviation Consumer Action Project (ACAP) lobbied then ultimately sued the FAA over the issue of requiring airlines to modernize in-flight medical kits. A federal appeals court ruled that the FAA did, in fact, have jurisdiction to mandate what should be in airline medical kits. So the FAA has the power right now; it can act to require auto-injectors in these kits.
Doing so would not be cost prohibitive. A 2019 study pegs the annual cost to the industry at $2.4 million – about 8 cents a year for each at-risk passenger.
It is time for the airline industry and those who oversee it to share responsibility for the safety of passengers with food allergies. Today, it’s estimated that an astounding 32 million Americans have food allergies. Yet I am fearful that it will take an anaphylaxis death in the air to prompt meaningful change.
Let’s not sit back and wait for that. There is an opportunity to address this issue now. Airlines must face the realities and responsibilities of treating life-threatening anaphylaxis in the air.
This opinion analysis is published exclusively for Allergic Living. Additional reporting by Gwen Smith. Lianne Mandelbaum is the founder of Nonuttraveler.com.
Related:
DOT Rules that Food-Allergic Child’s Rights were Violated
FARE Calls on Airlines to Urgently Stock Auto-Injectors on Flights
Petition: Revive “Airline Access to Emergency Epinephrine Act”





