 Photo: Getty
Photo: Getty First, Douglas Baker had a severe reaction in which he broke out into full body hives and lost consciousness three times. Then in a quest for answers, he went through nine long months of seeing a variety of specialists. During visits to an allergist, he was tested for more than 130 potential allergies, but to no avail.
The allergist could not identify the trigger that set off his life-threatening reaction and a few subsequent ones. Instead, the Huntsville, Alabama man got a frustrating diagnosis: “idiopathic anaphylaxis” or, as Baker calls it: “we ain’t got a clue.”
He was put on a heavy dose of daily antihistamines, instructed to always have epinephrine, never to be alone nor to stray more than 30 minutes from a hospital. The lifestyle was harsh but, for a time, his reactions waned.
Then in 2008, at the age of 62, the episodes came back with a vengeance. Over four years, Baker had 38 anaphylactic reactions, usually between 11 p.m. and 2 a.m.
Arriving at Hospital Unconscious
In some cases, he arrived at the hospital either semi-conscious or unconscious, even after getting epinephrine. Since doctors couldn’t figure out the cause, Baker was powerless to take action; he had no idea what to avoid. During one particularly severe reaction, in and out of consciousness with his throat swelling, he could tell the nurses and doctors were on edge. “I thought – this might be it for me,” recalls Baker, who was a soldier in the U.S. Army for 27 years.
As pressing as the fear of further reactions was, his desire to figure out what the heck was causing them was even greater. He was referred to well-known Memphis allergist Dr. Phil Lieberman, who got Baker into a National Institutes of Health study on idiopathic anaphylaxis.
 Over four years, Douglas Baker had 38 anaphylactic reactions with no known cause.
Over four years, Douglas Baker had 38 anaphylactic reactions with no known cause. In 2012, on a hunch, a physician working on the study tested his blood for alpha-gal allergy, a new condition. “She called me and said, ‘By the way, you should stay away from red meat.’” Seven years after his first big reaction, the veteran at last knew what he was allergic to.
It’s little wonder it took so long for Baker to discover the cause of his reactions. Hypersensitivity to galactose-alpha-1,3-galactose (aka alpha-gal) is a newly recognized condition, with the first U.S. case studies published in 2009. Called alpha-gal allergy or red meat allergy, it has turned what allergists thought they knew about food allergy on its head.
First, those with the condition create IgE allergy antibodies to alpha-gal, a carbohydrate or sugar that’s found in the meat of non-primate mammals, while other IgE-based allergic reactions are to proteins.
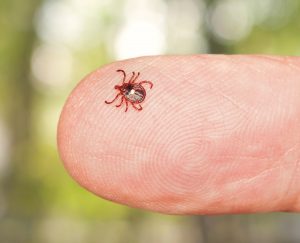
But where things get truly bizarre is the mode of sensitization to alpha-gal. It starts with a bite from a Lone Star tick (Amblyomma americanum), an insect attracted to deer as well as cows, dogs, wild turkeys and racoons.
The saliva from this insect appears to prime the immune system to react to red meat, including beef, lamb, venison and pork. Another break from traditional food allergy is that alpha-gal symptoms usually come on hours after eating red meat, as opposed to immediately, which makes the connection to the food less than obvious to the patient – or the doctor.
If the first challenge is diagnosis, the next is adjusting to a life without bacon, burgers, steaks and more. Baker is among the more sensitive alpha-gal patients who also have to avoid gelatin, which can appear in products from desserts to gravies and pills. He also can’t have most cheeses. For others, even dairy products such as milk can set off reactions.
The goal now becomes navigating a world of food avoidance, label-reading, questioning restaurant staff and carrying medication at all times. All from just the bite of a Lone Star tick.
Red Meat and Idiopathic Anaphylaxis
In short order, alpha-gal allergy has changed the very nature of adult allergy practices in the southeastern United States, as new research from Lieberman, Baker’s allergist, makes apparent. The condition is also increasingly showing up in more northerly regions and in children, too.
 Dr. Erin McGintee has seen more than 430 cases of alpha-gal allergy in her Long Island, NY practice.
Dr. Erin McGintee has seen more than 430 cases of alpha-gal allergy in her Long Island, NY practice. Since the 1990s, Lieberman’s team at the University of Tennessee allergy clinic has periodically published reports about the characteristics of anaphylaxis among their patient population.
In a 2006 report, Lieberman’s group found 59 percent of the clinic’s adult patients with anaphylaxis were diagnosed as “idiopathic,” an alarming rate that was still lower than the incidence in other U.S. research. But a review his team published in 2018 paints a different picture.
In an analysis of 222 cases of anaphylaxis between 2006 and 2016 among their clinic population – the incidence of idiopathic anaphylaxis had fallen 25 percentage points, to 34 percent. Why the big difference?
“We think the dent in idiopathic anaphylaxis was made by the discovery of allergy to alpha-gal,” says Lieberman. In the 2018 review, red meat allergy was seen as the cause in 32 percent of adult cases – a more frequent trigger than traditional food allergens. The longtime allergist thinks this condition has been going on ‘beneath our noses’ for decades. “I’ve heard over and over: ‘I woke up at 2 a.m., and I did have some meat at dinner,’” says Lieberman. But for years, “I’d never thought the association with the dinner was true.”
Lieberman’s clinic is in the heart of Tennessee deer country – Lone Star tick territory. Data from studies in high-risk areas peg the prevalence of alpha-gal allergy between 1 and 3 percent of the population. Better recognition of the disease shows it to be a growing issue in the east, and the aggressive tick is on the move.
It has traveled to some northern forests, which experts theorize relates to the rapid expansion of deer populations. There have been alpha-gal cases as far west as California, and north into Minnesota and Ontario, Canada. With the tick, comes the allergy.
 The red meat allergy diagnosis was life-changing for chef Matthew Beres.
The red meat allergy diagnosis was life-changing for chef Matthew Beres. Dr. Erin McGintee, an allergist in Southampton on Long Island, New York, diagnosed her first patient with alpha-gal allergy in 2010. The Lone Star population has surged on Long Island and today, McGintee has more than 430 cases at her practice.
“There are ticks everywhere here,” notes Matthew Beres, an East Hampton father of two, who is one of her patients. About six years ago, Beres got a red rash a few hours after eating a hamburger. After two more incidents, he went to see McGintee, who diagnosed an allergy to alpha-gal.
It was a life-changing moment for Beres, a personal chef. “I make all sorts of red meat products, so now I get someone to taste things for me. We get awesome beef from all over the world. It looks amazing,” he laments. For patients with higher sensitivity, it’s not as easy as just avoiding a steak, however. Beres reacts to many dairy products, as well as products made with gelatin, from jelly beans to certain medications.
Once, he had a severe anaphylactic reaction to a turkey sausage made with a pork casing. He still goes to restaurants, but grills them on how they cook the food – even a chicken breast cooked next to a steak could pose a problem. Once an avid beef eater, “Now I’m the guy with the portobello mushroom in his back pocket at barbecues.”
Related: Do You Have Red Meat Allergy?
Life-Changing Diagnosis
Madysen Bailey has similarly had her life changed by a Lone Star tick bite. The 17-year-old lives with her parents on a farm in Liberty, North Carolina, where ticks are a way of life.
“You get ticks from just walking to the car,” she explains. One evening in the spring of 2016, the teen was out with her mom, Maria, working on the farm, and had gone down to the barn to feed the horses. A while later she came to the front of the property to find her mom. “I think I’m dying,” Madysen said. She was hot, itchy and hives began to spread until she was covered from head to toe. Then she threw up.
Because Madysen had been outside at the time, the Baileys missed the connection to food, assuming her reaction was to fire ants, or some other insect. Maria took her daughter to an allergist and, after testing for insects came back negative, an astute nurse practitioner tested the teen for alpha-gal, which came back positive.
“It’s changed how we cook, she only feels safe eating at vegan restaurants, and we only eat our own food at potlucks,” says Maria Bailey. Last October, they took a road trip to Washington, D.C. and stopped at Mount Vernon, George Washington’s famous home. But on the way, Madysen shared some candy with her friend – a bite of a candy bar (that had milk in it) and three gummy bears.
“She went into anaphylaxis and I had to jab her with the EpiPen in the middle of George Washington’s historic home,” says the mom. “Now, when she’s looking at colleges, she’s making sure there’s a hospital close by. It’s amazing how this little tick has created this ripple effect.”
Why Do Some Become Allergic and Others Don’t?
It’s this ripple effect from the Lone Star tick that is keeping allergist Dr. Scott Commins busy in his lab at the University of North Carolina at Chapel Hill.
One of the things the leading researcher is trying to figure out is just how this tick prompts an allergy in humans, and why some people get it while others don’t. Because all non-primate mammals have alpha-gal in their blood, a prominent theory is that the tick needs to have fed on one of these mammals first, and then when it bites a human, the saliva transfers alpha-gal to the person, who then develops IgE antibodies to the carbohydrate. But another school of thought is that it doesn’t matter if the tick has fed on a mammal, but rather the tick just needs to bite the right “type” of person, and that person will develop an allergy.
“If that first notion is right, that the tick has to have fed on an animal, then it’s clearly not every tick, and that explains why some people get this and others don’t,” says Commins, an associate professor of medicine. But if it’s the second idea, “then you begin to think, ‘OK, I’m less worried about the tick, but what is it about the patient that responds to this?’” he says. It’s this type of information that can help Commins and his colleagues to direct their attention to areas that require more study, and eventually lead to a treatment for the allergy.
Another thing Commins and McGintee seek to understand is the delay from when a person eats the meat to when a reaction begins. It’s thought to have something to do with the way the body processes fat – and fattier foods, like burgers and ribs, are often the trigger in more severe alpha-gal reactions. From his studies, Commins has also started to think about this: If reactions to alpha-gal come on hours later, could other allergens work this way as well?
 Madysen Bailey with her mom, Maria.
Madysen Bailey with her mom, Maria. “Are there allergic responses to other foods that we’ve been missing because we’ve had too narrow a view?” asks Commins. He points to shellfish, and says it’s not uncommon to hear a story of someone who goes on vacation and eats a lot of shrimp, and then says they got a reaction in the middle of the night. In the past, the allergist would have brushed the shrimp association aside, but now he’s not so sure.
While the researchers toil in their labs, back on the farm, Maria Bailey misses her work buddy. Because there’s a chance Madysen’s allergy will go away over time if she avoids future tick bites, she doesn’t go outside as much.
“I don’t ask her to help me anymore. We’ve also gotten rid of our sheep, goats and pigs, because they carry ticks,” says the North Carolina mom. Madysen herself is trying to take the allergy in stride. She says she eats more vegetables now, and has “a whole lot more respect for others who have allergies.”
As for Baker, when he finally discovered what was causing his horrific reactions, he completely cut red meat out of his diet.
He credits his wife Jeannie for updating their menu. “She has discovered a wonderful turkey burger. She makes spaghetti, meat loaf and soup, all with poultry. And we eat a lot of fish.” He hasn’t had a reaction since. As a thank you, he sent coffee, doughnuts and pizza to the staff at his local emergency room, who had come to know him well. “I haven’t been down there in a while.”
Related Reading:
Do You Have Red Meat Allergy?
Meat Allergy Diagnosis: John Grisham a “Pro” at Managing Diet





