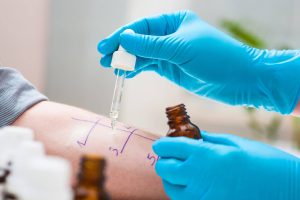
A team of allergists is urging improved standardization of allergen extracts used in allergy skin testing after studying peanut extracts that were recalled.
Their study of two of the recalled lots reveals the extracts, used in peanut allergy skin testing, contained either insufficient or no peanut allergens at all.
In December 2022, the U.S. Food and Drug Administration announced the manufacturer’s recall of four lots of peanut allergen extract vials. The recall came after allergists began reporting false-negative results with skin-prick tests. Some reported patients experiencing severe reactions after later eating peanut.
Dr. Cosby Stone says the FDA acted proactively and quickly on the recall. But after studying two of the recalled lots, he says improved standardization of allergen extracts is needed. This would ensure safe food allergy testing.
“This is a call to action,” he told Allergic Living. “With advances in technology, we can do better quality control,” says Stone, an assistant professor of allergy and immunology at Vanderbilt University Medical Center in Nashville.
In his team’s study, one recalled lot had 10 to 20 percent of the amount of peanut allergens that should be present. Meantime, peanut was “undetectable” in the other lot.
“The consequences of this are very serious,” notes Dr. Jonathan Hemler, who co-led the study. “Telling actual peanut-allergic patients they can eat peanut based on false-negative skin testing puts those patients in real danger,” says the pediatric allergist at the University of Virginia in Charlottesville.
The study followed Hemler’s firsthand experience. The recalled extracts threw off his UVA research team while they were conducting a clinical study that required peanut-allergic patients.
“Our team was using, unbeknownst to us at the time, a peanut skin testing extract that had essentially no peanut protein in it. We saw something was amiss right away,” Hemler says.
Unexpected Skin Test? What to Do
The UVA researchers noticed that patients with known peanut allergies and previous positive peanut skin tests were testing negative. When they received the recall notice, it confirmed their suspicions that those results were inaccurate.
“I can’t imagine what would have happened if we were using this peanut extract outside of a research setting, and clinical decisions were being made using the false-negative results,” says Hemler.
Since the recall, the FDA now requires all food allergen extracts to include warning labels about the risks of false-negative results and possible anaphylaxis.
Stone says false-negative test results are not common with food allergy skin-prick tests. But when they occur, they are challenging to discover. Physicians find out about false results if a patient has a reaction, or if they further investigate unexpected negative results. Extract lots with less allergen “can readily go undetected” in a clinical setting, according to the study.

That raises the concern, how would allergists know if they are using deficient allergen extracts to test patients?
Stone says if a patient with a known allergy suddenly has a negative skin test, a blood test can help confirm the result. A high result in a blood test with a negative skin test is cause for further investigation. This might be done with a skin test from another extract lot.
If an allergist notices several patients with false negatives from the same extract lot, it’s worth questioning, says Stone.
Patients with a negative test will often move forward to an oral food challenge, which involves eating specific amounts of an allergenic food. The goal is to see if the allergy has cleared. Stone says a patient who is concerned about a negative test can request a repeat test using extract from a different lot before trying an oral challenge.
One Extract Lot: ‘Undetectable’
For the study, published in The Journal of Allergy and Clinical Immunology: In Practice, the team compared recalled peanut allergen extracts against unrecalled extracts. The purpose was to determine whether a lack of peanut was behind the inaccurate test results.
First, in patients with known peanut allergies, they compared the size of wheal reactions (raised, often itchy bumps) during skin testing. They found smaller wheals from the recalled extracts.
The researchers then delved into the concentrations of the extracts of two recalled lots and three unrecalled lots. Their focus was on Ara h 1, Ara h 2, Ara h 3 and Ara h 6, the peanut proteins most responsible for reactions. (InBio, an allergy testing specialist company, also conducted the tests with similar results.)
The researchers then turned to monoclonal IgE antibodies, which were created from blood samples of allergic patients in a lab at Vanderbilt’s medical center. Study co-author Dr. Scott Smith finds B cells in the blood samples that generate the antibodies, which eventually create antibodies specific to the allergy patient, Stone explains.
Those antibodies were used to measure the amount of allergenic proteins in the extracts. That’s when they found the one lot of recalled extracts was devoid of key peanut proteins and the other had a significantly lower concentration than unrecalled vials, Stone says.
“I didn’t think it would be undetectable,” Stone says of finding the one lot lacked any peanut.
Updating Skin Test Quality Control
The use of monoclonal antibodies to measure allergens in this extract study is a first. Stone contends those antibodies could be similarly used to ensure quality control when measuring vials’ allergen content.
Currently, the FDA says that allergen extracts licensed for the diagnosis of food allergy in the United States are not standardized. So, it is up to extract manufacturers to test lots for allergen content.
The manufacturers test for proteins by “measuring the total protein concentration of a ground up food, pollen, or other allergenic substance,” according to the study.
But “total protein concentration” is not necessarily the same as the allergen content, Stone explains. “Allergens are not always just proteins, and proteins don’t automatically have allergens in them.”
Allergens are part of a protein’s structure that “stick out in a certain way and have a certain shape that a person’s immune system recognizes to say: ‘Uh oh! This is an allergen,’” Stone says. A patient’s immune system can elicit an allergic reaction when it recognizes those shapes.
But the protein could lose the detectable allergenic shape during manufacturing, Stone notes. Or, the wrong protein could be included from the source, such as ground-up peanut that might not contain the allergen.
That’s why Stone says using monoclonal antibodies to measure the allergen in the extracts with would be a major step forward for quality control. Manufacturers are already testing the lots, so they could use this more precise method instead, he says.
Hemler agrees monoclonal antibodies should be considered to improve standardization. “Improved quality control procedures are clearly needed in the manufacture of these extracts, so this doesn’t happen again.”
Related Reading:
Gut Microbiome Flaws Linked to Food Allergy, Eczema, Asthma
Study Finds OIT Can Lead to Remission in Peanut-Allergic Toddlers