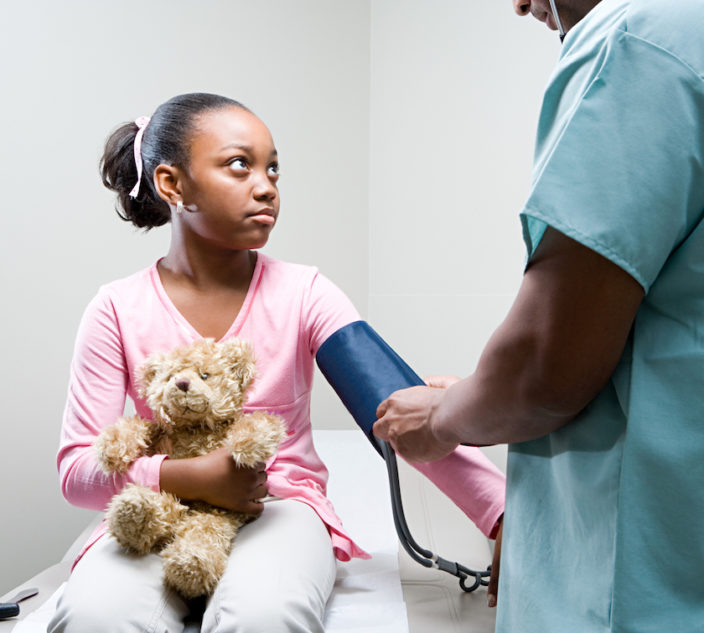
Milk and egg allergies primarily affect children. Children usually become allergic to milk and egg as infants or toddlers. So, there are extra precautions that need to be taken simply due to the age of the child. Very young children do tend to put everything within reach in their mouths, including their own hands.
This can present a challenge to parents who need to place a child in a daycare. While most licensed daycare centers are today well-versed in allergy issues (particularly peanut allergy). However, not all will be free of hard-to-avoid allergens such as milk and egg.
Before completing enrollment, make an appointment to review allergy practices of the daycare where you’re applying. Questions include:
– Can snacks be dairy-free or largely dairy-free (e.g. there are many brands of dairy-free crackers used as snacks)?
– What are the hand-washing practices following snacks and meals?
– What is the protocol for wiping down toys which are shared and could get smeared with, say, cheese residue?
Baked Milk and Egg Findings
Milk and egg are challenging allergies to learn to manage – because both are used extensively in packaged food and bakery items. But research shows that many allergic children are able to tolerate foods containing either milk or egg. What matters is that the foods have been cooked thoroughly at a temperature of 350 degrees F or higher. The amount of the allergen also is important.
Speak to your allergist about whether your child is a candidate for trying a baked goods challenge. (Never just try this at home on your own! Anaphylaxis is a risk). Research shows that many children tolerating thoroughly baked milk or egg can progress to foods that are less extensively baked. Examples are pizza or pancakes.
Managing Milk and Egg Allergies
Infant Challenges
Milk and egg allergies tend to appear in children before they reach the age of 3, so this presents a challenge. Many babies who become allergic to dairy have to switch to an extensively hydrolyzed formula that is considered “hypoallergenic” for those who react to cow’s milk.
International recommendations advise that soy formula not be given to infants under six months of age with cow’s milk allergy. For more on formulas to use with a child with milk allergy, see the advice of Dr. Hemant Sharma here.
Pay attention to breastfeeding with an infant with either milk or egg allergies as cow’s milk protein can pass through in breast milk and the same may happen with egg protein. But this doesn’t always happen and before you eliminate either one from your diet, speak to your doctor about your infant’s allergy. An allergist or pediatrician may refer you to a dietitian who specializes in allergies.
Hand-Washing: When your child (or you) has a milk or egg allergy, soap and water are your best friends. Hands should be washed thoroughly before and after eating. If you have a school-aged child, ensure he (or she) is able to wash his hands before snacks and lunch. With younger children, schools usually adopt an allergy protocol of washing hands among all children after eating.
Bring wipes with you at all times. They’re useful for cleaning hands, as well as wiping downs trays, tables and chairs when eating outside of your home.
Cross-Contact: It’s important to make sure milk or eggs or products with them don’t come in contact with the allergic child’s food. That means thoroughly cleaning utensils and kitchen equipment after use. For example, a family member might make a sandwich with egg-containing mayonnaise or a dairy-containing margarine. If so, be sure to clean the cutting board thoroughly with soap and water before using it for the allergic child’s food.
Label reading: The good news is that U.S. law requires the Top 9 food allergens (in Canada, it’s the Top 11) to be labeled in plain English. For more information on what you need to know when reading product labels, see “How to Read a Label with Food Allergies.”
However, labels are not always as clear as they’re meant to be. Whenever you eat a packaged food, do read the label in its entirety to check for any mention of milk or egg. Sometimes, they can have different names or can be hidden as an ingredient of an ingredient within a manufactured food. (Be mindful especially of supermarket foods made in-house. Not all deli and baking products fall under the allergen laws.)
You also have to look for precautionary warning statements on package labels, such as “May Contain Milk (sometimes “Dairy”),” or “May Contain Eggs.” These statements about foods that are not intentional ingredients are voluntary, so not all manufacturers include them.
In case of doubt: Contact the food manufacturer to find out whether there’s a risk of cross-contact with the allergen. If it’s an imported food and you cannot contact, always use the “when in doubt, go without” rule.
Speak Up About Food: With food allergies, you have to get over shyness or fear of offending. Whether grandma, a teacher or a server wants to serve food to your child (or you), you have to know if milk or egg are present.
It’s always nice when people try to accommodate your allergic child. However, if they are “99 per cent” sure a dish is allergy-friendly, you must consider it unsafe. It is far better to need to explain why you must decline rather than watch your child suffer a reaction.
It’s also important to teach an allergic child not to eat foods that others offer – unless mom or dad has pre-approved. When they’re older, they’ll need to know not to eat unless certain the allergens aren’t in the ingredients. For adults with milk or egg allergies, work to get past any embarrassment. Be certain to ask about ingredients, and learn to do this an efficient, confident manner.
At School: For a parent of a child with milk or egg allergies, sending them off to school can be a time of anxiousness.
It’s important to communicate clearly and calmly with your child’s teacher and the principal. As well, you’ll need anaphylaxis emergency plan to protect your child. For a child’s inclusion at school, experts usually recommend a federal 504 Plan (for U.S. children). Also ensure the teacher (and staff such as a coach) have training on using an epinephrine auto-injector and are aware where your child’s injectors are kept.
Be sure your allergic child knows not to share food with peers. As well, not to take food from anyone, including the teacher, unless you’ve said it’s OK.
At a restaurant: Dining out with a milk or egg allergy may seem daunting at first. But it is possible to do so safely and enjoyably. First, read a menu on the establishment’s website. Then call ahead to ask the manager or chef about menu items and their kitchen protocols to avoid cross-contact. If the chef or manager is unable to answer your questions or not aware enough, don’t eat there.
When you arrive at the restaurant, tell the manager and your server of your (or your child’s) serious milk or egg allergy. Discuss menu items that will be safe to eat.
Be mindful of particularly risky foods: sauces, desserts and salad dressings. Watch for dishes that are unsafe for you, which may be fried in the same oil as items that are safe for you. Some restaurants will be off-limits while others can be more reliable. For example, Italian and Greek restaurants tend to use olive oil rather than butter which can be safe for those with milk allergy. And remember: when in doubt, don’t eat it.
Be prepared: Make it a rule – no epinephrine auto-injector means no food. While you’ll do everything to make sure you’re not eating milk or eggs, accidents happen. Make sure you always have your auto-injector on you when you eat, in case of an emergency. If your child is allergic, make sure this rule is one he or she takes seriously.
Educating Others: In order to successfully manage a milk or egg allergy, those around you/your child need to be aware of the allergy and the serious consequences that could result from eating milk or eggs.
Plan what you’ll say to others to explain this condition. Be calm, clear about the information and keep the conversation based on facts. Politely request that they help you keep yourself or your child safe. You’ll often find that once a person understands about food allergies and anaphylaxis, they’ll be more than willing to help. Be mindful that there is a learning curve. So don’t expect people who don’t live with the allergy to absorb it all as quickly as you have.
Read More:
Food Allergies at School: The Steps to Ensure Your Child is Safely Included
Step-by-Step Guide to Dining Out with Food Allergies
Ages and Stages of Food Allergy Management